In 2018, First Script realized a 0.6% increase in generic utilization. 1 Generic medications contain the same active ingredient and approved indications as their brand name counterparts. An increase of 0.6% might not seem like a lot; however, when the difference in cost per script is considered, it is easy to see why a shift in favor of generic use is a win and can be a big cost saver.
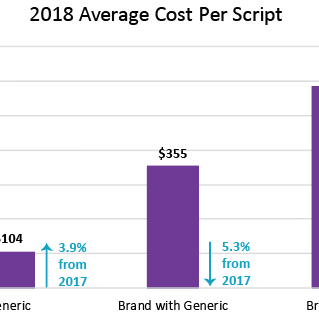
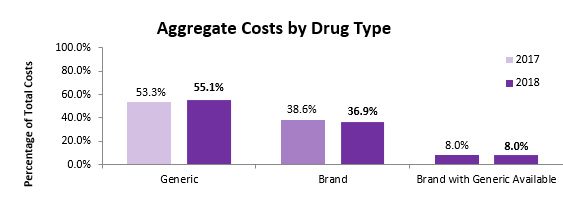
First Script’s average cost per script for a generic medication in 2018 was about $104. This is much lower than the 2018 average cost per script for brand-only and brand w/generic available medications ($584 and $355 respectively). A 0.2% increase in brand with generic available utilization was also seen in 2018. There are several reasons why a brand drug may be dispensed when a generic is available, the most common being at the request of the provider or injured worker. First Script uses step therapy rules, automated prior authorization messaging, outreach, and education in an attempt control the use of medications that fall into this category. It is worth noting that while the utilization in this group increased, the aggregate cost remained the same. 2 This is likely because the cost per script for brand with generic available drugs decreased from $375 in 2017 to $355 in 2018.
The most noteworthy shift in 2018, when speaking about brand and generic medication, is the 0.8% decrease in “brand only” utilization. We call it “brand only” to emphasize that the brand name drugs in this category do not have available generic alternatives. This decrease in utilization resulted in First Script spending 1.7% less2 on brand only drugs in 2018 than the previous year. One contributing factor to reduced brand only utilization is when drugs lose exclusivity. When a brand name drug loses exclusivity and generics are permitted to enter the market, shifts are to be expected, especially when it is a medication commonly seen in the workers’ comp world. For example, in 2017 buprenorphine patches (brand Butrans), a long acting opioid used to treat severe pain, was approved by the Food and Drug Administration (FDA). Subsequently, First Script saw more than a 30% drop in brand Butrans utilization in 2018 as compared to the prior year. Changes in utilization and cost of these drug types are affected by many factors. While First Script aims to control as many factors as possible and mitigate cost for our clients, we always keep the safety and health of the injured worker as a priority. To find out more about brand and generic drug trends, check out part two of the Coventry Drug Trends Infographic Series. In addition, be sure to stay tuned for additional posts like this one that address specific drug trends highlighted in the series, and if you miss an edition our series, please visit our Drug Trends Page.
1 Aggregate value includes First Script Retail, Mail Order and Out-of-Network Bill Review Clients
2 As a percent of total costs