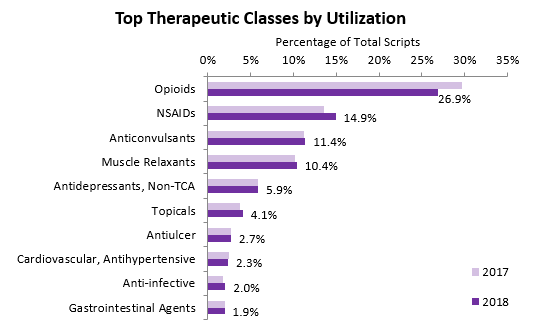
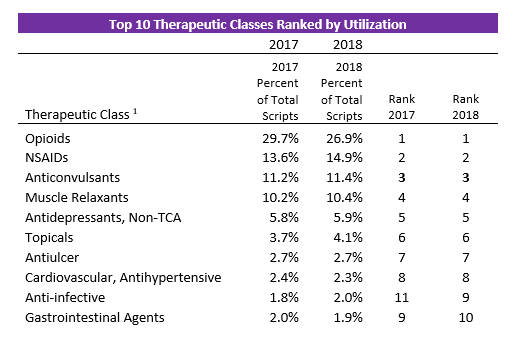
First Script saw a decrease in opioid utilization across our retail and mail-order programs in 2018. In 2017, opioids made up 29.7% of total prescriptions, dropping to 26.9% in 2018, and representing a 2.8% decrease in utilization year over year.
There are several factors that potentially contributed to this reduction. Such factors may include, early intervention into claims with opioid utilization, increased public awareness on the dangers of this therapeutic class, and an increase in the number of states placing restrictions on how these medications can be prescribed. Decreases in opioid utilization have led to a larger class share for five of the top six therapeutic classes. Non-steroidal anti-inflammatory (NSAID) utilization increased 1.3% and is the largest increase of the top 10 therapeutic classes. This non-addictive class of drugs can be used alone to treat pain and inflammation or along side opioids and other pain-relieving medications. It is encouraging to see NSAID utilization increase as it shows that safer, non-addicting alternatives are likely being used in place of opioids.
Anticonvulsants, muscle relaxants, non-TCA antidepressants, and topicals all showed smaller increases in utilization. These classes are commonly used with opioids to provide added pain relief, and potentially reduce the need for opioids. As with NSAIDs, a rise in these therapeutic classes is a positive shift because it may indicate adjunct therapy being used instead of escalating opioid treatment. As opioid utilization falls, there may be an increase in the number of prescriptions for non-opioid pain relief and opioid adjunct therapies such as NSAIDS, anticonvulsants, muscle relaxants, non-TCA antidepressants and topicals.
1 Opioid class Includes opioid dependence medications